Maximizing efficiency is a mission-critical goal for providers and payers alike. The vast amounts of data generated within the healthcare industry present both challenges and opportunities for strategists and organizational leaders. Because practice leaders and care providers are exceptionally busy, easy-to-understand, actionable analytics are the key to unlocking the potential for greater efficiency, cost savings, and improved patient outcomes at healthcare organizations of all sizes.
Leap Metrics’ Sevida helps providers and payers optimize operations by providing data-rich predictive and suggestive analytics and AI-driven care management workflows.
The Power of Predictive and Suggestive Healthcare Analytics
Healthcare analytics involves the systematic analysis of healthcare data to distill valuable insights, patterns, and trends. By harnessing the power of data, your organization can make truly informed decisions, streamline operations, and enhance the quality of care provided.
Predictive and suggestive analytics from Sevida’s AI-driven care management workflows provide next-best steps insights that your knowledgeable care team members can use to maximize productivity, evaluate contracts, and improve care delivery. Here are just some of the most insightful healthcare analytics reports available to improve efficiency:
- Population Health Management
- Identifying Health Trends: Analytics can identify population health trends, enabling healthcare organizations to allocate resources strategically and implement preventive measures to address emerging health issues for their members with special attention to priority populations.
- Social Determinants of Health (SDOH): Healthcare analytics can incorporate SDOH data to better understand the factors influencing health outcomes and develop targeted interventions. A comprehensive population health strategy requires factoring in SDOH for members. Sevida’s population health solution leverages analytics and AI to facilitate the unique needs of each healthcare organization.
- Risk Stratification
- Identifying High-Risk Patients: Healthcare analytics can stratify patients based on risk profiles. This helps healthcare providers allocate resources more effectively by focusing on patients with the highest risk of adverse health events, reducing hospital readmissions, and improving care coordination.
- Sevida Analytics stratifies members into risk groups, including rising risk, giving care managers and stakeholders insight into population needs and predictive cost of care estimates.
- Clinical Classification of members based on their diagnosis and risk profile also enables caregivers to proactively care for them, positively impacting outcomes.
- Quality Measures and Performance Improvement
- Sevida Analytics platform supports a wide range of quality measures from various measure stewards such as NCQA, CMS, States, and other entities.
- Sevida’s approach to quality measurement goes beyond reporting what happened and purports what might have contributed to the measure and what actions organizations should take at a member level to achieve their targets.
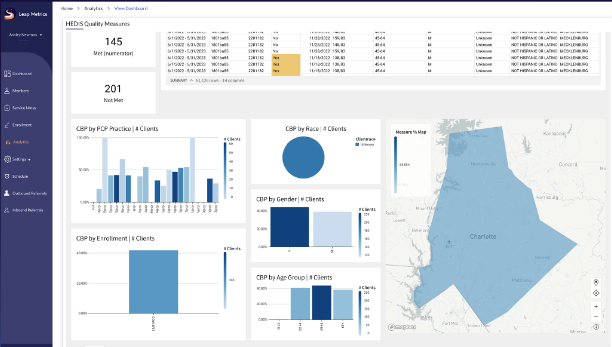
Sevida Quality Measures Dashboard
Sample measures Sevida supports include HEDIS (Healthcare Effectiveness Data and Information Set) and GPRA (Government Performance and Results Act). HEDIS is a widely used set of performance measures that assess the quality of care delivered by healthcare organizations. Healthcare analytics can help track and analyze HEDIS metrics, enabling organizations to identify areas for improvement and measure their performance against industry benchmarks. GPRA (Government Performance and Results Act) GPRA reporting is essential for federally funded healthcare programs. Analytics can assist in gathering, analyzing, and reporting GPRA data, ensuring compliance, and demonstrating the effectiveness of programs.
- Member Management
- Organizations receive member data from various sources and require a master data management strategy to eliminate duplication of records and shared member data. In most cases, lack of data sanity could result in loss of coverage for a member, causing serious consequences. Sevida Master Patient Index manages member data efficiently across multiple data sources, including the EHR, and tracks the lineage of data down to the field level, identifying and reporting discrepancies.
- The sanity of Member panels designated for care management is crucial to effective managed care. Data usually trickles down from the payers to the care management entity, causing data loss or corruption along the way. An effective solution like the Sevida platform is essential to catch data issues ahead of time and timely onboarding members on the panel.
- Patient Engagement: Understanding patient demographics, preferences, and historical data through analytics can enable more personalized and proactive care management, improving patient satisfaction and outcomes.
- Effective and timely management of changes in member circumstances, such as address changes and additions to a family, helps keep payers and providers in sync and provide quality care to members. Sevida member management workflows facilitate the capture and reporting of member changes seamlessly.
- Compliance Adherence
- Tracking Compliance Metrics: Healthcare organizations are increasingly required to report data and metrics to fulfill their value-based contracts, grant requirements, payer obligations, and other compliance needs.
- Proactive identification of gaps in compliance: Operations teams require proactive guidance on gaps in compliance to improve the quality of outcomes and maximize revenue. Predictive and prescriptive analytics offered by the Sevida platform prepare healthcare organizations for compliance proactively.
- Healthcare Compliance: Healthcare analytics that meet various regulatory requirements, such as HIPAA, ensure that organizations maintain the highest data security and patient privacy standards.
- Audit Preparedness: Analytics can assist in preparing for audits by providing comprehensive data records and demonstrating adherence to industry regulations.
- Billing Efficiency
- Value-based contracts tie payments to performance. Without technology that aligns payer contract rules with billing activities, providers and payers cannot survive. Sevida platform leverages its rule engine, AI engine, and Dashboards to support contract performance.
- Proactive rule-driven billing compliance insights are available as part of the Sevida AI-driven care management solution.
Today’s healthcare landscape is rapidly evolving from fee-for-service to value-based models, so maximizing efficiency is essential for delivering high-quality care while managing costs effectively. Sevida’s healthcare analytics and insights provide the tools necessary to achieve these goals. From quality measures and risk stratification to compliance adherence and billing efficiency, analytics are pivotal in optimizing every aspect of healthcare operations. Organizations require solutions like Sevida to view holistic member data through a single pane of glass that combines various facets of a member’s profile.
As healthcare organizations continue to embrace data-driven decision-making, the potential for improving patient outcomes and operational efficiency is boundless. By harnessing the power of healthcare analytics and AI, organizations can drive innovation, enhance patient care, and ultimately, empower healthcare to know enough to care for every life better.
See how your team can optimize efficiency with a customized demo.